- Home
- About
- Surgery List
- Squint Surgery
- Blepharoplasty
- Dark Circles
- Brow Droop:
- Ectropion
- Eyelid Tumours
- Facial Palsy
- Ptosis:
- Upper Lid Retraction:
- Trauma & eyelid reconstruction:
- Misdirected eyelashes (Trichiasis / Distichiasis):
- Watering Eyes
- Loss of an Eye & its Replacement Surgery:
- Entropion of upper or lower eyelids:
- A WATERY EYE
- Issues
- ISSUE 1.1 : VKC
- Issue 1.2 : Dry Eyes
- Guest Editorial – Dry Eyes
- Reference Articles – Dry Eyes
- Expert Lectures – Dry Eyes – Ocular Surface
- Expert Lectures – Dry Eyes – Understanding Dry Eyes
- Expert Lecture – Dry Eyes – Management of Dry Eye in Children
- Preparation – Dry Eyes – SERUM EYEDROPS (SED)
- Preparation – Dry Eyes – Acetylcysteine Eyedrops
- Preparation – Dry Eyes – Schirmer’s strips
- Preparation – Dry Eyes – CYCLOSPORIN E/D
- Case Report
- Pearls
- Videos – Dry Eyes – Clinical Assessment of a patient with Dry Eyes
- Videos – Dry Eyes – Assessing the Tear-Film BUT
- Videos – Dry Eyes – Schirmer’s 2 Test
- Videos – Dry Eyes – Schirmer’s 1 Test with Anaesthesia
- Videos – Dry Eyes – Schirmer’s 1 Test without Anaesthesia
- Issue 1.3 : Microbial Keratitis
- Patients
- Updates
- Lectures
Clinical Updates
“My Child is Squinting his Eyes”

Fever is a sign that there is an infection somewhere in the body. Similarly, squinting of eyes also indicates that something is wrong with the child’s eyes and it is mandatory to find the cause of the squint rather than having it corrected surgically.
Remember “SURGERY IS NOT THE TREATMENT OF A SQUINTING EYE BUT A LAST RESORT”.
Human eye is like a camera. It gathers light impulses from the objects and transmits that information to the brain which then analyzes the details of that image. Remember there are two cameras (eyes) operating side by side. If the information transmitted by one eye is hazy or blurred, the brain gets confused. It blocks the faulty information from the problematic eye and that eye starts to squint i.e. turns inwards or outwards. The eye conditions that lead to a squint are:
1) Droopy upper eyelids.
2) Clouding or haziness of the cornea or lens of the eye.
3) Gross short-sightedness or far-sightedness.
4) Retinal or optic nerve malformation.
The most common cause of a squinting eye in children is far-sightedness. The child needs glasses to see clearly. Failure to recognize and rectify this problem with correcting glasses makes the child squeeze his eye muscles which then turn the eye inwards.
Whenever this problem is noticed, the help of a pediatric ophthalmologist should be sought urgently before that eye loses its sight permanently.
Surgery for such an eye is not the answer as it can only straighten the eye for a short while but cannot restore the sight. An eye with poor vision will soon deviate again.
“How Do I Know My Child Needs Glasses”
Young children usually cannot understand or complain that they cannot see clearly. If this problem is not diagnosed early and correcting glasses are not given timely, a child starts neglecting his work at school, his writing becomes bad and his performance in class drops. Gross near-sightedness reduces a child’s horizon as he can see clearly only up till a meter or a two meter distance hence he starts losing interest in outdoor activities which demand a good distant vision; he becomes more inclined towards indoor activities and becomes a loner.
As a parent, we can diagnose that the child needs glasses by keeping a look out for the following symptoms:
1) Frequent blinking or rubbing the eyes.
2) Squeezing both eyes to see at a distance object.
3) Closing one eye while a photograph is being taken or outdoors.
4) Watching T.V standing close to it.
5) Worsening of hand writing and performance at school.
6) Squinting of one eye while reading or looking at a distance.
7) Watering of eyes while watching T.V or outdoors.
If you notice any of these symptoms, please see a pediatric ophthalmologist who is especially trained to recognize this problem and rectify it. Longstanding neglect of a child’s poor vision results in a “lazy eye” which is difficult to treat.
Amblyopia can be treated successfully at all ages
According to my recent clinical research at a tertiary referral center in Lahore, Pakistan, dense amblyopia was successfully treated in 195 children and adults between age 13 – 45 years (median 15 years). Their visual acuity improved from 6/60 to 6/6 Snellen’s after 2 months of full-time occlusion therapy and near visual activities for 3-4 hours per day.
It is important to realize that an amblyopic eye is not a dead eye but a lazy, sleepy eye; the brain connections lie dormant because of an inhibitory influence of the good eye. Once this inhibition is removed, the sleepy eye wakes up.
This therapy only works if the patient compliance is excellent.
Only highly motivated and inspired patients will comply to the therapy and will regain good vision,
 02 Jun 2013
02 Jun 2013
Cyclosporin Eye Drops: A magical steroid-sparing drug
Cyclosporin Eyedrops are an effective therapeutic agent in the management of a variety of autoimmune diseases especially ocular surface disorders like vernal keratoconjunctivitis, dry eye syndrome, mild to moderate anterior scleritis, VKC, Mooren’s Ulcer, Neurotrophic Corneal Ulcer, Corneal Melting.
Mechanism of action: Cyclosporin is a new class of drug that appears to work by inhibiting cytokine production by immune cells (T lymphocytes) and interfering with the action of interleukin-2 (as in scleritis, Mooren’s ulcer, Dry eye syndrome). IgE mediated immediate hypersensitivity response as in VKC. Studies support the efficacy of topical cyclosporine treatment through its immunomodulatory action, reversing inflammation of the ocular surface and lacrimal glands.
Animal studies have shown that Cyclosporin has no intraocular penetration; it concentrates on the ocular surface which enhances its anti-inflammatory effect after long term use. Even after a year of regular topical therapy, none to minimal blood concentration is found in rabbits.
Rationale of using varying concentration of eyedrops: Cyclosporin eyedrops can be prepared in varying concentrations depending upon the severity of the ocular surface disease; if the inflammation is marked, then 1-2% concentration should be used, 3-4 times /day; gradually the strength and frequency is reduced according to the clinical improvement.
Preparation of eyedrops: Cyclosporin capsules are available in 25mg and 100 mg strength (Sandimum neural: Novartis) which contain a water miscible gel.
- To make 1% concentration, take gel out of two 25 mg capsules by a disposable syringe, put it in a sterile eye drops bottle and add 5 ml distilled water. Shake it well and dispense.
- For 2% concentration, take either one 100 mg capsule or four 25 mg capsules and mix their gel in 5 ml
- For 0.5% concentration, take one 25 mg capsule + 5 ml distilled water.
- For 0.05% concentration, take one 25 mg capsule + 10 ml distilled water.
Indications:
- Mooren’s ulcer, Severe VKC, severe scleritis, corneal melt: 2%
- Moderate Scleritis, moderate VKC, Stevens Johnson’s syndrome: 1%
- Dry eyes: 0.5 – 0.05%
 27 May 2013
27 May 2013
A STEPWISE APPROACH TO DRY EYE
Concept of A LACRIMAL FUNCTIONAL UNIT (LFU)
It comprises of the lacrimal gland, Ocular Surface and a Neural Network to provide a feedback from ocular surface to the lacrimal gland. Only that amount of tears are produced as are required by the ocular surface, depending upon the information sent to the lacrimal gland through the neural network.
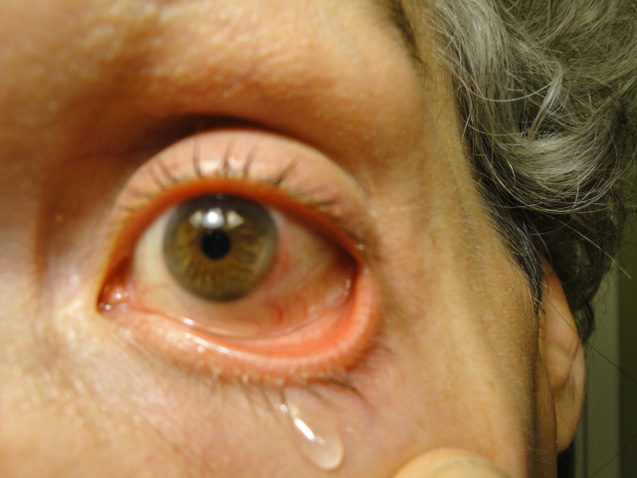
Pathogenesis of dry eye: A multifactorial disease. Either it results from reduced tear production with increased tear osmolarity & an inflamed ocular surface. Or increased tear evaporation due to deficiency of lipid layer. Or poor wetting of ocular surface causing dry, damaged corneal epithelium. Even in presence of adequate tear production.
Lipid layer deficiency: due to meibomian gland dysfunction → Tear evaporation.
Aqueous layer deficiency: in KCS which is divided into: SS (Sjogren’s Syndrome) as in RA, SLE, Multiple sclerosis and Non-SS KCS: in pregnancy, postmenopausal women, HRT
Mucin deficiency: Stevens Johnson syndrome, chemical burn, Trachoma, Ocular cicatricialPemphigoid → Poor Wetting of Ocular Surface.
Predisposing Factors for Dry eye:
Old age: usually seen in post-menopausal women.
Connective tissue disorders
LASIK : lifting of corneal flap damages corneal nerves.
Drugs: beta blockers. antihistamines, AGT.
Diabetes: Type 2, impaired autonomic innervation to lacrimal gland, reduced corneal sensitivity, poor lac. Gland microvasculature, advanced glycation products activated cytokines.
Vitamin A deficiency
Effects of Ageing:
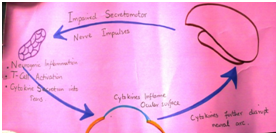
Ageing causes androgen deficiency. Estrogen & androgen receptors are present in the lacrimal & meibomian glands. Androgens are trophic for lacrimal & meibomian glands. They are potent anti-inflammatoryagents ( TGF beta) & suppress lymphocytic infiltration of lacimal glands. Androgen def. causes inflamed lacrimal and meibomian glands, with tear def. & hyperosmolar tears. These cause a pro-inflammatory environment on ocular surface. Also cytokine production and T-cell activation further inflame ocular surface, disrupt the neural arc.
Cytokines inhibit neuronal function. They convert androgens to estrogens and increase the level of tissue degrading enzymes
MANAGEMENT OF DRY EYE
It is a STEP-WISE APPROACH. It is important to listen to patient’s symptoms, find and eliminate the predisposing factors and find and treat the cause. Simply prescribing artificial tears does not work. This is an ocular surface disease; unless a wetting surface is restored, loading the eye with tear drops is useless.
Smptoms: Burning, Blurring of vision,Photophobia,paradoxical tearing.All symptoms are worsened by smoking, reading, computer work. Find the predisposing factors by a careful history.
Examination: aim is to find the cause resulting in a dry eye and to grade its severity. Grading decides the step-wise management and helps in assessing improvment on follow-up.
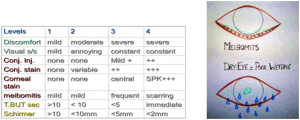
Grading of Dry Eye: according to symptoms & signs
LEVEL 1: LEVEL 2:
1: Environmental & dietary modification Pt. symptoms don’t improve, T BUT &Schirmer =/< 10
2: Eliminate the cause. Add: Anti-inflammatory therapy:
3: Artificial tears. steroids, CsA, omega 3 fatty acids, Tetracyclines
4: Eyelid therapy. Punctal plugs
Tetracyclines: antibacterial, anti-inflammatory, antiangiogenic, reduce lipase production→ FFA→stabilize tear film.
CyclosporinA : increases aqueous &meibomian sec., increases goblet cell count, decreases cytokines & inflammatory cells in conj.
LEVEL 3: LEVEL 4:
If symptoms are severe, conj. & central corneal staining; Severe symptoms, SPK+++, conj
TBUT & Schirmer< 5mm Scarring/symblepharon, TBUT
Permanent punctal occlusion immediate, schirmer<2mm :
Autologous serum Systemic immunosuppressant drugs.
Soft contact lens Surgery: amniotic or mucus membrane graft, lid surgery, tarsorrhaphy
Autologous Serum: Contains trophic factors which promotes growth & migration of epi. cells. immunoglobulins, vitamins & are non-antigenic. Containdications; HIV, Hepatitis B, anaemia. Complications: bacterial keratitis, conjunctivitis, scleral vasculitis & melting.
FOLLOW-UP
1) Note subjective improvement.
2) Check the status of lid margins, cornea, tear meniscus.
3) Perform Schirmer’s test & TFBUT every visit to gauge efficacy of therapy.
4) NOTE: 3 layers of tear film; 3 tests to diagnose the abnormality of tear film.